 Nearly 60 million Americans suffer from arthritis. However, most people don’t realize that there are nearly 150 forms of it. The forms range from degenerative arthritis (osteoarthritis); soft tissue (bursitis and tendonitis); autoimmune arthritis (rheumatoid arthritis, lupus); joint infections, crystal arthritis (gout; pseudogout); reactive arthritis (psoriatic arthritis); to metabolic bone disease (osteoporosis). As our population ages, the public health costs of arthritis to the public as well as affected families are staggering. Osteoarthritis, a wearing out or loss of articular cartilage in joints, affects 43 million people in the United States.
Nearly 60 million Americans suffer from arthritis. However, most people don’t realize that there are nearly 150 forms of it. The forms range from degenerative arthritis (osteoarthritis); soft tissue (bursitis and tendonitis); autoimmune arthritis (rheumatoid arthritis, lupus); joint infections, crystal arthritis (gout; pseudogout); reactive arthritis (psoriatic arthritis); to metabolic bone disease (osteoporosis). As our population ages, the public health costs of arthritis to the public as well as affected families are staggering. Osteoarthritis, a wearing out or loss of articular cartilage in joints, affects 43 million people in the United States.
Osteoarthritis (OA) exists in all races and creeds in several forms and results from chronic inflammation or irritation, hormonal imbalances, heritable or developmental defects and trauma.
Osteoarthritis, a wearing out or loss of articular cartilage in joints, affects 43 million people in the United States. |
A variety of factors such as increased age, obesity, certain occupations associated with kneeling or squatting, muscle weakness, alterations in bone mass, and medications such as corticosteroids are additional predisposing factors. Although OA can be found in any of the joints in the body, it is most commonly found in the hip, knee, hands and feet. The most common symptoms are pain, stiffness, swelling, achy muscles or joints, fatigue weakness or deformity often accompanied by discomfort with motion, swelling, abnormal posture or gait, crepitation (crunching sounds on movement), color changes and limited stamina or endurance. The presence of OA is usually suggested on a physical examination carried out by a doctor, and confirmed by characteristic findings of joint X-rays.
The direct and indirect costs of managing the 23 million Americans with OA totals 149 billion dollars a year and constitutes 2.5 percent of our gross national product. It is in some way responsible for 744,000 hospitalizations a year representing 4 million days of in-patient care. Though two-thirds of people with OA are over 65 years of age, it affects 44 percent under 65. OA is the second most common cause of disability in the United States (and most common after the age 65) and 5 percent of the workforce retires as a result of it each year. This adds up to 68 million days of missed work and 95 billion dollars in lost wages annually. There are 100,000 Americans who can’t even walk to the bathroom independently due to hip or knee OA.
The management of OA is multifaceted. Patients are educated on how to help themselves, improve their coping skills, get a good night’s sleep, enhance their social support system, lose weight and eat a healthy diet. Moist heat alleviates joint discomfort, stretching exercise programs protect joints. Physical therapy and occupational therapy help people with OA assess their activities of daily living, employ concepts of energy conservation and joint protection, instruct in the use of assistive devices, maximize work capacity and minimize pain.
For mild OA, acetaminophen (Tylenol) is the drug of choice along with the occasional use of ibuprofen (Advil) or aspirin for intermittent symptoms. Patients with chronic, ongoing moderate symptoms benefit from anti-inflammatory regimens such as selective cox-2 nonsteroidals (Celebrex, Vioxx), non-narcotic analgesics (Ultracet) and local steroid injections. Occasionally, topical salves with aspirin-like ingredients, capsaicin, camphor or menthol are useful as is injections of hyaluronan into severely degenerative knees.
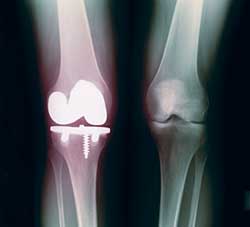
Nearly 14 billion dollars is spent annually on alternative approaches such as chiropractic, herbs and acupuncture with varying degrees of success. More than 300,000 Americans have knee or hip surgery each year, most of them involving the replacement of damaged joints.
There is light at the end of the tunnel. What can we look forward to over the next few years? From a medicine standpoint, improved and safer aspirin-like derivatives are already in clinical trials. Agents which block newly understood pain pathways that turn out to amplify OA pain (the NMDA pathway) are being developed. Three new families of medicines are being tested for OA: drugs which block an enzyme which destroys cartilage, called metalloproteinases, growth factors which promote the growth of new cartilage, and cytokines, which signal the bone to influence cartilage. From a surgical standpoint, not only are new and improved joint replacement options becoming available, but several new, innovative approaches are being studied. These include harvesting cartilage and transplanting it into a joint, transplanting bone, and developing new biomaterials (gels, glues, carbon fiber matrices) which will act like cartilage. Hopefully, by the year 2020 when 60 million American with have OA, musculoskeletal specialists will have an improved armamentarium to help suffering associated with this disease.

