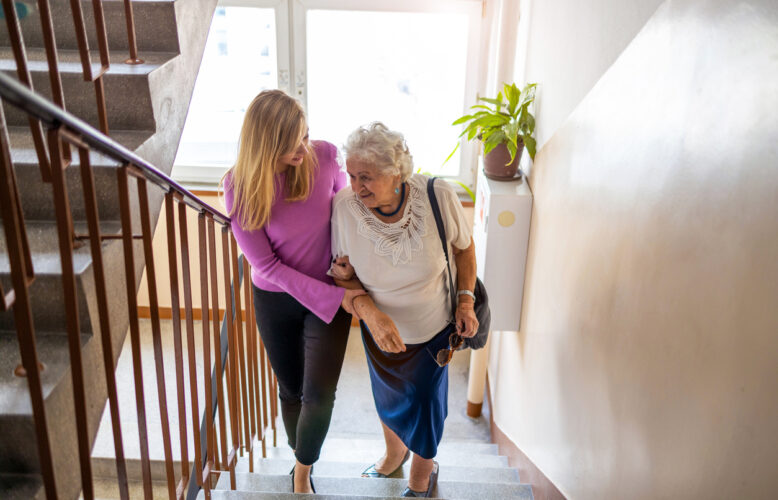The Centers for Medicare & Medicaid Services (CMS) has announced its final coding, benefit category, and payment determinations for seat elevation on Complex Rehab Technology (CRT) power wheelchairs. But the agency is putting off its final coding and funding decisions for seat elevation on consumer power chairs. The CRT determinations were included in CMS’s Second…
Feature Stories See More >
CMS Pauses Group 2 Seat Elevation Coding, Funding Decisions
Why Cardinal Health ‘Wants to Be a Major’ Enabler of At-Home Care
Rob Schlissberg, president of Cardinal Health’s at-home business, looks forward to 2024.
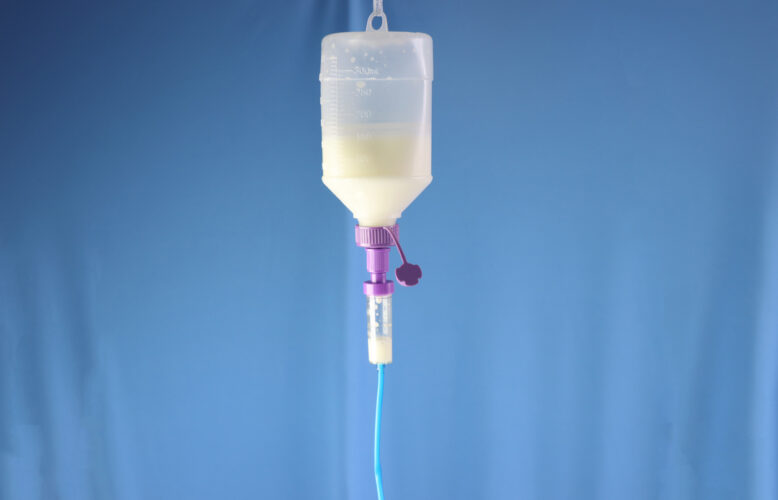
NHIA Releases Practice Standard for Home Infusion Electronic Mechanical Pumps
New standard provides guidance to home infusion stakeholders.

Study: Caregivers’ Health Is Poorer Than Health of Non-Caregivers
U.K. study cites the mental and physical toll of taking care of others.

CMS Releases Details of Lymphedema Compression Treatment Coverage
Medicare coverage starts Jan. 1, 2024.
Legislative See More >
AAHomecare: Final Push Needed for S.1294/H.R. 5555 Support
Advocates are asked to reach out to their Senators and Representatives.
The American Association for Homecare (AAHomecare) has asked industry members to reach out to their Senators and Representatives on behalf of bills S. 1294 and H.R. 5555, which would extend the 75/25 blended rate for home medical suppliers in non-competitive-bidding areas. In a Dec. 13 announcement, AAHomecare noted that H.R. 5555 was approved by the…
House Energy & Commerce Health Subcommittee Approves Two HME Bills
H.R. 5555 and H.R. 5371 now proceed to the full Energy & Commerce Committee.
NCPA Supports Senate PBM Bills
The Better Mental Health Care, Lower-Cost Drugs, and Extenders Act was passed by the Senate Finance Committee last week.
NHIA Submits Home Infusion Comments to Congressional Committees
The association noted how home infusion can improve outcomes while saving money.

AARC Reports Successful Annual Respiratory Fly-in
Advocates attended more than 200 meetings on Capitol Hill.
Today on HME Business
Briefly: VGM Launches Post-Acute Playbook; Apria Answers Patients’ Questions
Featuring VGM & Associates and Apria Healthcare Group.
VGM Launches Post-Acute Homecare Playbook VGM & Associates has introduced a new playbook, “Perspectives on the Next Generation in Post-Acute Homecare.” In an April 16 news announcement, VGM said the new publication “provides a succinct view on the next generation of the industry.” “Innovations and evolutions of technology, services, products, software, and even customer experiences…Change Healthcare Fallout: CMS Shares Payer Resources
New document provides information and tips for specific payers in the cyberattack aftermath.
As the health-care community continues to suffer billing and payment delays following the February cyberattack on Change Healthcare, the Centers for Medicare & Medicaid Services (CMS) released a list of resources for providers. “CMS has passed along a 35-page document with resources related to the Change Healthcare cyberattack disruption and contact information for United Health…AdaptHealth Names HME Vet Suzanne Foster New CEO
Foster replaces Chairman Richard Barasch, who had been filling the role on an interim basis.
AdaptHealth Corp.’s (Nasdaq: AHCO) search for a new CEO is over. Earlier this month, AdaptHealth announced that Suzanne Foster is stepping in as the company’s top executive. AdaptHealth had been looking for a new CEO since Stephen Griggs vacated his post last summer, with Chairman Richard Barasch filling the role on an interim basis. “Our…Q1 Most-Read: The Industry’s Future Takes Center Stage
The most popular HME Business stories from January through March had a common theme.
The three most-read HME Business stories of Q1 2024 featured some of the biggest names in the home medical equipment (HME) industry, and hinted at what the future could hold for those companies and the industry at large. Why Cardinal Health ‘Wants to Be a Major’ Enabler of At-Home Care, written by Joyce Famakinwa, featured…CDC Report: Pharmacies Were ‘Integral Partners’ During COVID-19 Pandemic
Study details the ability of pharmacies to reach communities across the country.
A new report from the Centers for Disease Control (CDC) confirmed what pharmacy personnel and their customers surely already knew: Pharmacies that participated in the Federal Retail Pharmacy Program (FRPP) “served as integral partners in national efforts to scale up vaccination capacity during the COVID-19 pandemic emergency response.” Published in the Morbidity and Mortality Weekly…DME MACs Announce HCPCS Code Updates for April
Power seat elevation codes are among this month’s changes.
The Durable Medical Equipment Medicare Administrative Contractors (DME MACs) have released HCPCS code updates for durable medical equipment and Complex Rehab Technology equipment, effective April 1. In an April 12 bulletin, CGS Administrators — the Jurisdiction B and C DME MAC — listed the following updates: A4271: Integrated lancing and blood sample testing cartridges for…VGM Announces Changes to Member Success Team
The member services organization announced a promotion and a new hire.
VGM & Associates has announced an addition and a promotion to its member success team. In an April 10 press release, VGM said Chris Rose had been promoted to director of member key accounts, effective April 8. Rose, who was previously a regional account manager, will now “focus on strengthening business relationships between members and…Fisher & Paykel Launches Nova Micro Nasal Pillows Mask in New Zealand
New mask will be available in the United States and Canada later this year.
Fisher & Paykel Healthcare has given obstructive sleep apnea patients another potential choice in masks. In an April 9 news announcement, the manufacturer introduced its F&P Nova Micro nasal pillows mask to its home country of New Zealand, while adding that the mask will be introduced in Canada, Australia, Europe and the United States later…Briefly: Inogen to Report Q1 Earnings; Rebound Medical Reports Growth Investment
Featuring Inogen, Rebound Medical Systems, and Castleford Capital.
Inogen to Report Q1 Earnings on May 7 Inogen will host a conference call to report its 2024 first-quarter financial results on Tues., May 7, at 5 p.m. Eastern. Attendees in the United States can call (877) 841-3961 to listen in. Attendees outside the U.S. should dial (201) 689-8589 to join the conference call. Inogen,…Computers Unlimited Receives SOC 2 Type II Attestation
The attestation was the result of an independent audit conducted by KirkpatrickPrice.
Computers Unlimited has received SOC 2 Type II attestation after completing an independent audit conducted by KirkpatrickPrice, an information security auditing firm. In an April 11 news announcement, Computers Unlimited, based in Billings, Montana, said the attestation “provides evidence that Computers Unlimited has a strong commitment to security and to delivering high-quality services to its…People in HME See More >
AdaptHealth Names HME Vet Suzanne Foster New CEO
Foster replaces Chairman Richard Barasch, who had been filling the role on an interim basis.
AdaptHealth Corp.’s (Nasdaq: AHCO) search for a new CEO is over. Earlier this month, AdaptHealth announced that Suzanne Foster is stepping in as the company’s top executive. AdaptHealth had been looking for a new CEO since Stephen Griggs vacated his post last summer, with Chairman Richard Barasch filling the role on an interim basis. “Our…
VGM Announces Changes to Member Success Team
The member services organization announced a promotion and a new hire.
VGM Group Adds Two Board Members
The new board members replace VGM co-founders John Deery Jr. and Jim Walsh.
Tomorrow Health Bolsters Growth Team with Key Hires
The expansion comes as the company works to capitalize on the significant demand for high-quality home-based care.
Joel Marx Honored As Homecare Champion
The award was presented at the Stand Up for Homecare reception last week.
Accreditation See More >
The Compliance Team Celebrates 30th Anniversary
The celebration kicked off at last week’s Medtrade.
The Compliance Team (TCT) is celebrating “30 years of optimizing health-care delivery and patient outcomes with their proprietary Exemplary Provider Accreditation and Certification Programs,” the company said in a March 26 news announcement. The 30th anniversary commemoration was a focal point of TCT’s booth at Medtrade, which took place in Dallas, March 26-28. A more…
Briefly: Inogen to Report Results; ACHC Updates Hospice Standards
Featuring Inogen Inc. and the Accreditation Commission for Health Care.
BOC Announces Public Member Appointment
The new appointment currently serves as Senior Manager Payor Relations at Coloplast.
BOC Creates Lymphedema Accreditation As CMS Begins Coverage
The Lymphedema Treatment Act final rule went into effect on Jan. 1.
BOC Seeks Nominations for Certificant of the Year
Nominations are open through Feb. 12.
COVID-19 See More >
CDC Report: Pharmacies Were ‘Integral Partners’ During COVID-19 Pandemic
Study details the ability of pharmacies to reach communities across the country.
A new report from the Centers for Disease Control (CDC) confirmed what pharmacy personnel and their customers surely already knew: Pharmacies that participated in the Federal Retail Pharmacy Program (FRPP) “served as integral partners in national efforts to scale up vaccination capacity during the COVID-19 pandemic emergency response.” Published in the Morbidity and Mortality Weekly…
Competitive Bidding See More >
House Committee Passes Amended Version of H.R. 5555
New version excludes the 90/10 blended rate adjustment for suppliers in former CBAs.
An amended version of H.R. 5555, the DMEPOS Relief Act of 2023, has been approved by the U.S. House Energy & Commerce Committee, the American Association for Homecare (AAHomecare) has announced. In a Dec. 6 announcement to stakeholders, AAHomecare said the amended version of the bill “extends the 75/25 blended rate in non-CBAs [competitive bidding…
Oxygen See More >
6 Key Quotes from HME Executives That Capture Market Trends
Executives shared their comments during recent earnings calls and industry meetings.
The home medical equipment (HME) market is experiencing massive change, from technology innovations and skyrocketing demand, to shifts in how payers operate. Sometimes, the market moves so fast that it’s difficult to read the headwinds and tailwinds. Recent comments made by industry executives during company earnings calls and investor presentations, however, shed light on critical…
Briefly: Inogen to Report Results; ACHC Updates Hospice Standards
Featuring Inogen Inc. and the Accreditation Commission for Health Care.
CAIRE Opens Global Service Headquarters in Georgia
The new home base is near CAIRE’s Atlanta manufacturing hub.
AAHomecare Launches Market Impact Survey
Briefly: CRT Awareness Week, Cardinal Health’s Upcoming Dividend, COPD Research
Pain Management See More >
Sales & Marketing See More >
Sleep Therapy See More >

Q1 Most-Read: The Industry’s Future Takes Center Stage
The most popular HME Business stories from January through March had a common theme.
The three most-read HME Business stories of Q1 2024 featured some of the biggest names in the home medical equipment (HME) industry, and hinted at what the future could hold for those companies and the industry at large. Why Cardinal Health ‘Wants to Be a Major’ Enabler of At-Home Care, written by Joyce Famakinwa, featured…
Fisher & Paykel Launches Nova Micro Nasal Pillows Mask in New Zealand
New mask will be available in the United States and Canada later this year.
6 Key Quotes from HME Executives That Capture Market Trends
Executives shared their comments during recent earnings calls and industry meetings.
Samsung: FDA Authorization of Galaxy Watch Feature Will Drive Sleep Apnea Detection, Care
New feature will be available in the United States later this year.
Quipt Home Medical CEO Touts Long-Term Tailwinds, M&A Track Record
CEO and Chairman Gregory Crawford addressed stakeholders during his company’s 2024 fiscal first-quarter earnings call.
Software & IT See More >
NikoHealth Launches Electronic Medical Attachments Feature
New feature is designed to improve HME providers’ operational efficiency.
NikoHealth’s latest innovation is improving the synergies between home medical equipment suppliers and funding sources. In a Nov. 28 announcement, NikoHealth launched its Electronic Medical Attachments function, which the company said is “revolutionizing the way durable medical equipment (DME) suppliers interact with insurance payers.” The “game-changing” new functionality “allows DME suppliers to submit essential attachments…